

Get new exclusive access to healthcare business reports & breaking news




Illinois residents who received the one dose Johnson & Johnson COVID-19 vaccine have become worried recently, because of the more contagious delta variant which emerged, and want to get a shot of a Moderna or Pfizer vaccine, hoping it will increase their protection.
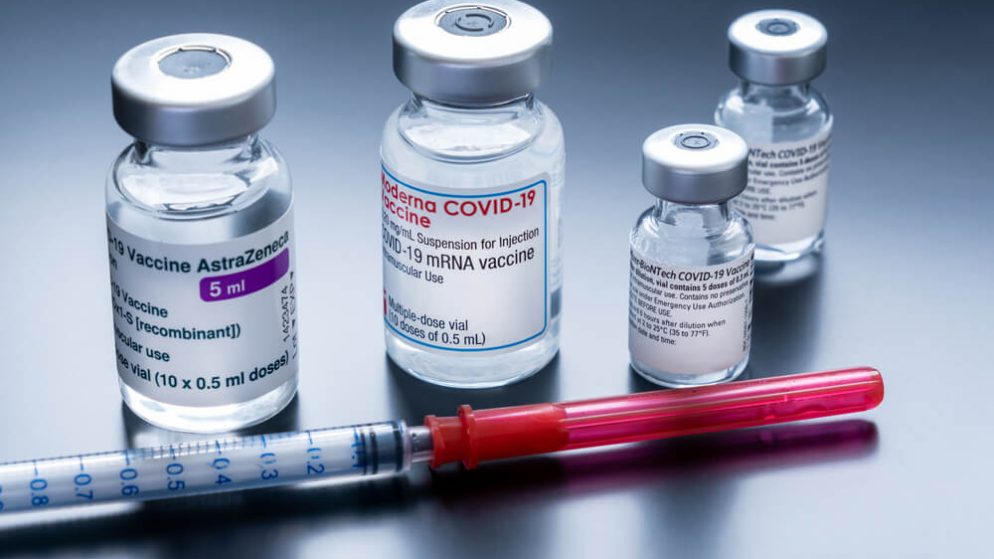
The Johnson & Johnson vaccine was found to be 66% effective at preventing COVID-19, while Pfizer and Moderna were 95% and 94%, respectively, although all three were found to be highly effective at preventing hospitalization and death from the illness.
J&J said last January the vaccine was 85% effective in preventing severe disease and Covid-related hospitalization four weeks after vaccination in all adults. “We’re proud to have reached this critical milestone and our commitment to address this global health crisis continues with urgency for everyone, everywhere,” J&J CEO Alex Gorsky said in a statement.
The Centers for Disease Control and Prevention and most experts are not recommending that people who received Johnson & Johnson vaccines, or any other vaccine, get booster shots. People are wondering however if a booster is not a good idea, a good idea, especially since some experts publicly recommended it and it is already done in other countries. There are people who ask their doctors for advice on the matter, others who are taking things into their own hands, and have already gone to local pharmacies and gotten Moderna and Pfizer vaccines, after being previously vaccinated with Johnson & Johnson shots.
Both CVS Health and Walgreens say they follow CDC guidance, but is there really a way of knowing if a person asking for a vaccine has already been vaccinated? Illinois’ largest health insurer, Blue Cross and Blue Shield of Illinois, said it isn’t aware of any claims for vaccines being denied because the second dose of a vaccine came from a different manufacturer than the first.
According to doctors, there is no reason to get boosters for Johnson & Johnson vaccines now, especially for healthy people under 65, who have more likely developed antibodies. Following CDC guidance might be in their own interest, since consequences of getting a Pfizer or Moderna vaccine on top of Johnson & Johnson remain unknown. Dr. Michael Angarone, an associate professor in the department of medicine and division of infectious diseases at Northwestern University Feinberg School of Medicine, thinks caution is a good idea.
“We know that vaccines are not without side effects,” Angarone said. He worries about side-effects especially in people with autoimmune diseases, since extra doses of vaccine could worsen the symptoms of those illnesses. “I think when we don’t know the benefit, and we know there’s potential risk, in my mind, that is a risk I don’t think we want to put people under.”
Overall, inoculating as many people as possible should be the main focus, since general vaccination reduces the risk of infection, and those already inoculated are having at least some degree of protection. Good news came for parents, since the U.S. Food and Drug Administration (FDA) has okayed the use of Pfizer-BioNTech COVID-19 vaccine on adolescents aged between 12 and 15 years of age on an emergency use basis, a move that is aimed at the safe reopening of schools in the fall.
Still, there is a divide even between specialists since, in recent weeks, several prominent health experts made headlines for publicly encouraging people who received Johnson & Johnson to get Moderna and Pfizer shots.
Dr. Vin Gupta, a faculty member at the Institute for Health Metrics and Evaluation at the University of Washington and an NBC News analyst, tweeted late last month that people who got Johnson & Johnson should get a Moderna or Pfizer shot as a booster. Dr. Angela Rasmussen, a virologist at the Vaccine and Infectious Disease Organization at the University of Saskatchewan, also tweeted last month that she got a Pfizer vaccine to “top off the J&J vaccine I received in April.”
The makers of all three vaccines say they offer protection against the delta variant though Pfizer has said it plans to ask the U.S. to authorize a booster.
Many people have also been looking at what other countries are doing with booster shots.
Last month, Canada’s National Advisory Committee on Immunization said that a first dose of the AstraZeneca vaccine should be followed up with a dose of Pfizer or Moderna, partly to elicit a better immune response. A similar recommendation has been made by specialists in Germany.
Though the AstraZeneca vaccine is not the same as the Johnson & Johnson vaccine, they rely on similar technology.
Experts don’t seem to get on the same page about recommending boosters for the general population, but even those who do not think everybody should get another dose are recommending boosters for certain patients. Basically, as the flu shots, which are different for elderly people, to help them stimulate their immune system enough to not catch the disease, different health situations could impose different approaches when it comes to supplementary Covid vaccines.
Dr. Mia Taormina, chair of the department of infectious disease at DuPage Medical Group, said she has recently recommended Pfizer or Moderna shots to patients who had already gotten the Johnson & Johnson vaccine but were immunosuppressed and didn’t develop antibodies after getting it.
Doctors and health experts are waiting for more data to help them determine who, if anyone, needs boosters. For individuals, the wait is more difficult to endure, especially since the delta variant is spreading, now comprising more than half of new COVID-19 cases in the U.S., with only 288 known cases in Illinois mid July.