

Get new exclusive access to healthcare business reports & breaking news




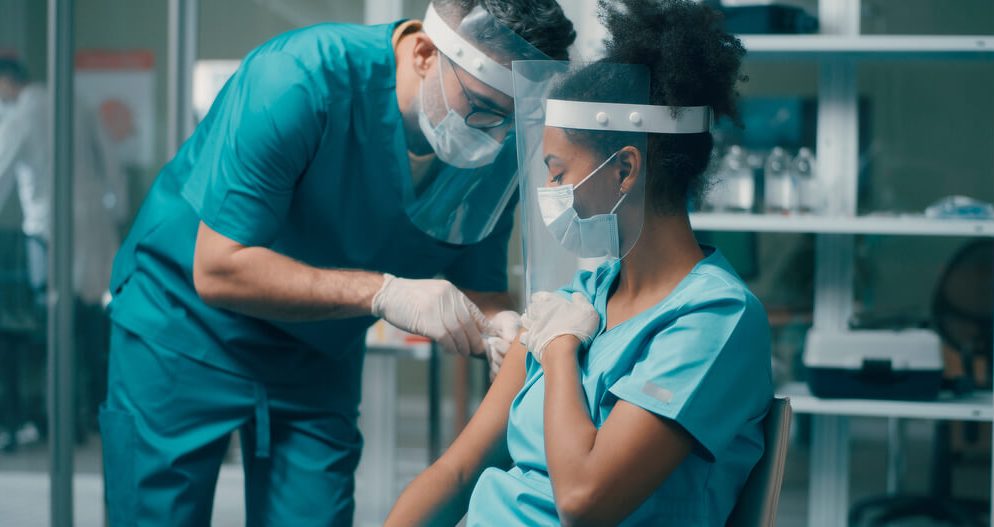
All the major hospital systems in the Chicago area have mandated COVID-19 vaccination for their staff members, Northwestern Medicine being the last one to do so for its 23,000 workers statewide.
This is good news for all the vaccinated people needing medical care, because taking all precautions at home and workplace, while finding out you are exposed exactly in the place you least expected to be is not an experience we need or desire, especially now, that Delta variant COVID-19 cases are more and more frequent. So, the fact that Northwestern Memorial Hospital completes the circle of major hospitals in the area which have required vaccinations, as urged since July by medical national and international organizations, is good news for everybody.
“Given the spread of the COVID-19 Delta variant and its risk to those with underlying medical conditions and children under 12 who are not yet eligible to receive a vaccine, Northwestern Medicine physicians and staff will be required to complete COVID-19 vaccination or receive a medical or religious exemption by October 31,” a Northwestern Medicine statement said.
Northwestern announced their decision a day after AMITA Health, one of Illinois’ largest health systems, transformed a voluntary compliance policy into an obligatory one and mandated vaccines for its 20,000 employees statewide by Nov. 12.
The urge to issue vaccine mandates for healthcare staff members had come from more than 50 medical groups nationwide, as soon as the Delta variant started to spread rapidly among the unvaccinated. The hope was that the FDA approval of Pfizer-BioNTech’s COVID-19 vaccine would persuade holdout hospitals and health systems to demand vaccinations since this vaccine type was considered to be more efficient. Illinois residents who received the one dose Johnson & Johnson COVID-19 vaccine have become worried when the more contagious delta variant emerged and wanted to get a shot of a Moderna or Pfizer vaccine, hoping it would increase their protection.
The Johnson & Johnson vaccine was found to be 66% effective at preventing COVID-19, while Pfizer and Moderna were 95% and 94%, respectively, although all three were found to be highly effective at preventing hospitalization and death from the illness.
J&J said last January the vaccine was 85% effective in preventing severe disease and Covid-related hospitalization four weeks after vaccination in all adults. “We’re proud to have reached this critical milestone and our commitment to address this global health crisis continues with urgency for everyone, everywhere,” J&J CEO Alex Gorsky said in a statement.
The continued work on the various types of vaccines opens up some new business opportunities, with healthcare industry companies trying to get into the game. Danaher Corporation has announced that it has entered into a definitive agreement to acquire Aldevron from EQT Private Equity for an enterprise value of $9.6 billion. Aldevron will operate as a standalone operating company and brand within Danaher’s Life Sciences segment.
Aldevron manufactures high-quality plasmid DNA, mRNA, and proteins, serving biotechnology and pharmaceutical customers across research, clinical and commercial applications. Aldevron’s custom manufacturing capabilities enable scientists and biotech companies to develop and supply new breakthrough genetic medicine, and Aldevron has played an important role in combating COVID-19 by supplying plasmid DNA used to manufacture mRNA vaccines.
“We are thrilled to have Aldevron join Danaher’s Life Sciences segment. For nearly 25 years, Aldevron has made tremendous contributions to the advancement of cell, gene, and other novel therapies and vaccines. This acquisition will expand our capabilities into the important field of genomic medicine and help us support our customers and their critical mission to bring more life-saving therapies and vaccines to market faster,” said Rainer M. Blair, Danaher President, and Chief Executive Officer.
AMITA, NorthShore University HealthSystem, and Northwestern Medicine were the last major hospitals to issue the mandates, all other significant hospitals in the area have already done so. Before AMITA, NorthShore issued, mid-August, an Oct. 31 deadline for its 18,000 workers to be vaccinated.
Basically, if healthcare workers do not get vaccinated, they will have to suffer consequences, varying from suspension without pay up to and including termination of the contract. It is either get jabbed or get jobless, but vaccinations as a prerequisite of employment, with varying degrees of consequences — ranging from suspension without pay, up to and including termination.
The debate over imposing vaccination for healthcare workers has been rampant, one side arguing freedom of choice and the fact forcing people to get vaccinated might increase an already critical health care workforce shortage — if those workers choose to leave rather than be vaccinated.
On the other side, groups including the American Medical Association, American College of Physicians, American Nurses Association, and American Public Health Association have backed compulsory vaccination as the fulfillment of health care workers’ “ethical commitment” to take all steps necessary to ensure patients’ health and well-being.
The hospitals will attempt to accomplish full compliance, by watching closely the response of reticent workers. Some are more lenient than others, though. Northwestern, for example, is allowing unvaccinated workers to get tested weekly after Oct. 31 and will wait until Jan. 1, 2022, to begin taking more radical measures concerning employment.
Northwestern, which has 10 acute-care hospitals, had earlier implemented voluntary compliance, arguing 75 percent of its workers were vaccinated. That figure is now at 80 percent.